|
|
Post by Ken & Fergie on Jul 26, 2021 6:56:13 GMT -7
[Original subject line:Neck Pain and Root Signature ]
Hello everyone,
My 10 year old 65 lb American Bulldog has been healthy all of his life. He had a dental cleaning with Xray done [7/19] 7 days ago and when he got home, he was noticeably in discomfort. He started yelping in pain, which I thought was a sore mouth. But it persisted. He has been having intermittent episodes of yelping, usually when he is in a sleeping position and when he is trying to get up.
I believe he has a slipped disc in the neck when under anesthesia during his dental procedure. Here are my observations:
1. The first day he got back, he yelped, rear leg gave out a bit, and lied down immediate with an arched back. But return to normal a min later.
2. A majority of the time, he yelps when he is in a sleeping position or trying to get up. He has yelped when walking and when I tried to lift his chin up.
3. Most of the time, he is able to move his neck freely. But during an episode, he would yelp once loudly, head is lowered, tail tugged, I believe right shoulder muscles tremor, right front leg lifted, sometimes he would walk restlessness.
4. He is willing to go on walk and seem to be fine. He is able to pee lifting his legs. He's appetite is normal.
5. I massage his neck and spine but he is not bothered by it at all.
6. I believe he is now anxious and moves gingerly. He lies down more.
What stage of IVDD is he and is root signature considered neurological involvement?
I have contacted the vet and was told to put him on restricted activity for 2-3 weeks if pain is the only symptom. I asked for pain meds and got Galliprant 60mg once a day. He's been on it for 2 days now but he is still yelping. He will be examined by the vet again later today.
[Moderator's Note. Please do not edit
65 lbs 10 y.0.
Galliprant as of 7/19: 60mgs 1x/day for ? days, then TEST STOP for _ pain/_neuro
needs GI tract protector, Pepcid AC, on board w/Galliprant! ]
Things I am doing now:
Restrict movement as much as I can, though the neck is difficult.
No stairs, I carry him up and down to potty with a leash.
Elevated bowls.
Light massages with heat compress.
I truly appreciate any help and advice that I can get. Thank you!
|
|
PaulaM
Moderator.    Member since 2007: surgery, conservative . Montana, USA
Member since 2007: surgery, conservative . Montana, USA
Posts: 19,528
|
Post by PaulaM on Jul 26, 2021 8:31:43 GMT -7
Welcome to the Forum. Hi, my name is Paula, what's yours and your dog's? It well appears there has been damage to a neck disc. Neck discs can cause pain and could affect both the front and the back legs. Dental anesthesia puts neck and trunk muscles which support the vertebrae to sleep sleep. Extra things you can do for a neck disc: More info here: dodgerslist.com/2020/05/05/cervical-care-tips/How to execute single most important care: STRICT rest: dodgerslist.com/2020/05/14/strict-rest-recovery-process/Do what you can at potty time to limit to only minimal footsteps (no walking around) to take care of business. LARGE DOGS: If your dog is too big too carry with safety it is still important that the amount of movement to the potty place be minimized to only a very few footsteps. --Try a pee pad right outside and adjacent to the crate. --Add caster wheels to a wire crate and wheel down ramp over steps to outside. -- place crate near sliding glass door, to provide minimal footsteps onto a potty place on the deck. Potty spot could be some dirt, sod, snow). -- IF potty place is on your deck, use combo of white vinegar and water in a watering can to cleanse. Vinegar takes away the smell of urine as the acity kills bacteria. ⚠️White vinegar can kill grasss/landscaping if you have 'em under the deck. PAIN signs Resolution of spinal cord inflammation/swelling provides the relief from pain. It can take an anti-inflammatory (steroid or a non-steriodal NSAID) a range of 7 to 30 days before all swelling is gone. Galliprant was designed and targeted specifically for swelling pain of arthritis. Normally with a neck disc the most powerful anti-inflammatory of steroid like prednisone or a broad spectrum NSAID would be used. PROBLEM: a switch from Galliprant would require TWO stomach protectors on board for the double jeopardy of not doing a 5-7 days washout from Galliprant Powerhouse anti-inflammatory meds do wonders OR they can be dangerous. Vets who practice safe medicine and owners up to speed on medications make all the difference. Answers here:
The best pain medications control is using more than one approach to address pain from multiple fronts (traMADol-general analgesic, methocarbamol- muscle spasm pain, gabapentin-nerve pain). All three pain meds need to be prescribed three times a day. i.postimg.cc/N0YM7022/Crate-transport-vet-diagnosis-CHUNK.jpg Transport to a vet involves risk of too much movement of the spine with potential to then damage the early healing disc, especially with a large dog. The benefits of the treatment need to be weighed against the risk of too much movement. IF an exam is necessary to get the meds, then pad out the crate with rolled up blanket or towels snuggly around your dog. This prevents shifting of the neck or back as you take a corner or come to a stop. When you get to vet, phone them you have arrived so someone can help you safely carry your dog into the exam room.
There should be no sign of pain from one dose of meds to the next. Have no patience with pain as it does hinder healing. Look for your dog to be acting their normal, perky self when pain is fully under control round the clock.
SIGNS OF PAIN: ⚙︎ shivering-trembling ⚙︎ yelping when picked up or moved ⚙︎ tight tense tummy ⚙︎ arched back, ears pinned bac ⚙︎ restless, can't find a comfortable position ⚙︎ slow or reluctant to move in suite such as shift positions ⚙︎ not their normal perky interested in life selves ➕if a neck disc: ◻︎ head held high/ nose to the ground ◻︎ looks up with just eyes and does not move head and neck easily. ◻︎ not eating due to painful chewing or in too much overall pain ◻︎ holds front or back leg up flamingo style not wanting to bear weight
Avoid touching/massage the neck/spine. Pain meds properly Rx'd would give full comfort from pain.
Let us know what the vet diagnosis, the meds Rx'd, etc. |
|
|
|
Post by Ken & Fergie on Jul 26, 2021 16:15:13 GMT -7
Thank you so much. My name is Ken and my dog's name is Boyboy.
I did get ✙Gabapentin 300mg 2-3x per day and continue Galliprant 60mg once per day.
My vet did not give me a diagnosis. He only referred me to a neurologist. If I am not considering surgery yet, there is no rush to see a neurologist, is that correct? Or is there something that the neurologist can detect that the regular vet cant?
[Moderator's Note. Please do not edit
65 lbs 10 y.0.
Galliprant as of 7/19: 60mgs 1x/day for ? days, then TEST STOP for _ pain/_neuro
✙Gabapentin 300mg which actually giving 2 or 3x/day?
needs GI tract protector, Pepcid AC, on board w/Galliprant! ]
When there is root signature sign, does that mean there is nerve involvement? And prognosis is not as good? A ER vet said it might take 4-6 weeks, so how do I know if the disc defect is healing? Does it happen gradually? If within that 4-6 weeks, he is still yelping. What should I do?
If he yelps, does that mean the nerve is being injured more and thus delaying healing?
Does neck brace work? like the one below?
https: //alpha-mobility.com/shop/balto-dog-neck-brace-bt-neck/
Also, are there any supplements that promote healing?
Thank you.
|
|
PaulaM
Moderator.    Member since 2007: surgery, conservative . Montana, USA
Member since 2007: surgery, conservative . Montana, USA
Posts: 19,528
|
Post by PaulaM on Jul 26, 2021 18:36:54 GMT -7
Ken, glad you now have one source of pain being covered, that of nerve pain with the gabapentin. Since pain meds last for about 8 hrs, that is the reason to dose promptly every 8 hrs. Please let us know how often you are dosing so we have the correct med list info. What about the other 2 sources of pain and managing them promptly every 8 hrs? Very typical to a neck disc is muscle contraction pain that is managed with the pain med methocarbamol. Often an overall analgesic is Rx'd as well a synthetic opiod, traMADol Not all vets know IVDD. So they rightly refer to a higher authority a specialist: a neuro (ACVIM) or an ortho surgeon (ACVS). There are many general family DVM vets who do know IVDD. There may be one in your town. An appt with a neuro or ortho is because your local family DVM vet is not comfortable with using the typical pain meds used with a disc episode, not comfortable in their knowledge of IVDD. So seeing a specialist is not just for the sole purpose of a surgery. When/if you should make an appt, be sure to note the reason you are seeking an appt. Since you do not have a diagnosis, until you get one, it would be prudent to act as if this might be a disc episode on the premise of not further damaging the neck disc which in turn could compress the spinal cord to cause neuro function loss. A disc episode with conservative treatment of 8 weeks of very strict rest to heal the disc can only proceed if proper pain meds can be brought on board to provide round the clock and dose to dose pain relief. MONITOR nerve function loss As damage to the spinal cord increases, there is a predictable stepwise deterioration of functions. When nerve healing begins, often it follows the reverse order. 1. √7/26 Pain caused by the tearing disc & pain of inflammation in the spinal cord and peripheral nerve: Yelps, right front leg not weight bearing; head lowered, 2. Wobbly walking, legs cross 3. Nails/toes scuffing floor 4. Paws knuckle under 5. Weak/little leg movement, can't move up into a stand 6. Legs do not work at all (paralysis, dog is down) 7. Bladder control is lost. Leaks on you when lifted. Can no longer sniff and then pee on that old urine spot outdoors. 8. Tail wagging with joy is lost 9. Deep pain sensation, the last neuro function, a critical indicator for nerves to be able to self heal after surgery or with conservative treatment. If surgery is not an option (for whatever reason) then the best option is conservative therapy. Surgery can still be successful in the window of 12-24 hours after loss of deep pain sensation. Even after that window of time, there can still be a good outcome. Each hour that passes decreases that chance. Precious hours can be lost with a local DVM vet that gets DPS wrong. Trust only the word of a neuro (ACVIM) or ortho (ACVS) surgeon about DPS. So if surgery is an option for your family get to a neuro or ortho asap. A quick overview of conservative treatment vs. a surgery: dodgerslist.com/2020/02/10/surgery-vs-conservative/A disc episode compresses the spinal cord and causes a lot of bruising, swelling, and painful inflammation. -- Surgery immediately relieves the pressure by removing offending disc material where it is not supposed to be -- Conservative treatment relieves pressure with an anti-inflammatory drug and takes 7-30 days.
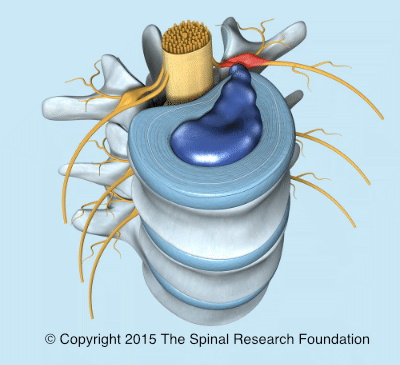
Boy is a good candidate to heal under conservative treatment IF pain can be fully in control. Just as with any traumatic injury, the body can self heal nerve damage and self heal the disc. -- The disc heals under Conservative treatment with very STRICT limited movement and time of 8 weeks. -- Damaged nerves in the spinal cord self heal with time after a surgery or conservative treament. Best to think in terms of months rather than days/weeks for this slowest part of the body to heal. -- Full comfort from pain happens in 1 hour or less when the right combo of meds, dose and Rx'd every 8 hrs happens. -- Inflammed spinal cord tissue heals with the aid of a broad spectrum NSAID or a steroid such as prednisone. The NSAID Galliprant was designed to target only the pain of arthritis read package insert for yourself, so may not be the best choice for the more typically painful neck discs. PROBLEM as noted in my previous post, to switch another NSAID or to the steroid class (such as prednisone) would require not just Pepcid on board as it should have with start of Galliprant, but adding a 2nd ( SUCRALFATE) due to double jeopardy Galliprant taking 5-7 days to leave the body while the new anti-inflammatory starts. Please post on your fridge the "Conservative Road Map." The map goes over all these details to keep you safely on a good path during conservative treatment. Here is the link to d/l and print out: dodgerslist.com/wp-content/uploads/2020/07/Roadmap-for-Fridge.pdfROOT SIGNATURE PAIN (if you get that diagnosis from a vet) The Veterinary Specialists of Rochester: This Bagley article is written for veterinarians. Excellent information, if you have patience for the technical vocabulary: www.scribd.com/document/23748101/CANINE-Lateral-and-Foraminal-Disk-Extrusion-in-Dogs?ad_group=5982&campaign=VigLink&content=27795&irgwc=1&keyword=ft500noi&medium=affiliate&source=impactradiusDog is in pain and won't bear weight. Holds leg like a flamingo bird i.postimg.cc/764Q46mk/flamingo-bird-Thumb.png **Here is what the nerve root being pressured by the bad neck disc looks like. The spinal cord is a bundle of nerves. Nerve root exiting the cord, is being painfully pinched by escaping disc material (dark blue). root signature illustrated © Copyright 2015 The Spinal Research Foundation. All rights reserved. Ken, it is important that you get a diagnosis. There are other diseases that can mimic the symptoms of a disc episode. The treatment of any of the other disease could be very different than the necessary VERY STRICT rest for a disc episode. Until you have that diagnosis that says this is not a disc episode, it is prudent to act like this is a disc episode. Please keep us updated. We are anxious that pain is not being properly managed for a disease Boy may have and is known to be quite painful. |
|
Marjorie
Moderator~    Member since 2011. Surgery & Conservative
Member since 2011. Surgery & Conservative
Posts: 5,724 
|
Post by Marjorie on Jul 27, 2021 5:10:03 GMT -7
To answer your question about neck braces, should this be an IVDD episode (and you must treat it as such until you receive a different diagnosis in order to protect the spine), we don't recommend using braces. Dodgerslist has consulted with professionals about braces. Here is what the consensus was. -- Braces do not prevent a future disc episode. Disc disease is the cause of prematurely aged discs. A disc problem happens at the point the disc has hardened too much. -- Can cause muscle atrophy in the spine which is the support for the vertebrae -- Discomfort or anxiety by having to wear it, hard to get on a dog who is even slightly painful if during a disc episode -- Must monitor for pressure (rub) sores Put simply, there isn't enough research on them for us to support their use. What we do know is that strict crate rest is what works - it's proven. We like *sure* tried and true things that we know to be safe. Orthotics like a back brace should require an Rx from a board certified neurologist (ACVIM) who is well educated in disc disease, just the same as any reputable company would require. An ill fitting product that is not custom made can do more harm. Here's our page with information on supplements and braces: dodgerslist.com/2020/02/24/devices-supplements/Knowledge is the best defense in fighting IVDD. So do keep any questions or concerns coming and please continue to keep us updated. Healing prayers for Boy. |
|
|
|
Post by Ken & Fergie on Jul 27, 2021 10:25:33 GMT -7
Boyboy does not seem to be painful unless he moves a certain way, ie lifting his head while in a sleeping position. He can manipulate his head no problem and walk fine, lift up legs to pee, etc.
It is difficult to keep his neck from moving. Can it still heal?
I am considering surgery if he does not get better in 6-8 wks.
I wanted to avoid CT and Xray. Usually MRI and surgery will suffice, is that correct?
I need to schedule an appt with a neurologist now because they are all booked out for months.
How do I know which is recommended? I live in the SF Bay Area.
Also is 300mg of Gabapentin every 8 hrs too much for a 65lb dog? Boyboy just seems sleepy all the time.
My vet did give me Methocarbamol but do not suggest all 3 meds at the same time unless I consult with a neurologist.
I noticed Boyboy seems to have muscle twitches in his neck and rear legs when he's sleeping-- is that related to IVDD?
Thank you.
|
|
PaulaM
Moderator.    Member since 2007: surgery, conservative . Montana, USA
Member since 2007: surgery, conservative . Montana, USA
Posts: 19,528
|
Post by PaulaM on Jul 27, 2021 11:43:30 GMT -7
Ken, simply put, IF you observe pain signs then he has pain that is not yet under control. Best to say what you observe rather than just saying he is painful. Helps a vet and helps us to best understand things. You can browse the Forum, to see each dog's med list. Vet's who know iVDD meds whether they are family DVM vets or specialists, understand the reason behind a multi-modal approach of using multpile meds on board at the same time. Each med deals with a different source of pain. Why would one not want to treat all sources of pain? There is no one size fits all mg doses. It is you working with the vet you hire, giving feedback about being too sleepy with 300mgs 3x/day. Your vet may then advise try 200mgs 3x/day, advocate for it if vet does not. You will see 17lbs doxies taking 200 mgs 3x/day in addition to traMADol and methocarbamol. Each dog can react to differently to differing doses in mgs, so it is testing out the dose to get it right for your dog. The reason for every 8 hrs is that is how long these pain meds stay in the body til excreted. When a multi-model pain med approach is on board, the dose in mgs is adjusted for the individual dog's needs for pain relief to get it just right. Again it is you working with your vet to report how his Rx's are working. Can you call around to sound out another potential DVM vet hire you can get help from, if your vet just is not comfortable in learning what you have learned to give it a try for full pain relief? I know my own vet will pick up the phone to call a colleague at a nearby university to fill in his learning gap when needed. That is what good vets do when there is a waiting list for month to see a specialist!
Best Friends Vet explains to dog owners: Dr. Pancotto ACVIM (Neurology) writing for veterinarians: The reasons for considering a surgery are: --- vet has Rx'd an aggressive pain med approach but pain can't be fully brought under control round the clock/dose to dose. So far your vet is very light on use of pain meds!!! --- After several courses of 7-day or 14-days courses of a broad spectrum NSAID or a steroid, the swelling will not resolve. It may take 7-30 days for the anti-inflammatory to resolve all swelling. IF the anti-inflammatory can't, then a surgery would be a consideration. ADVANCED IMAGING MRI's are the gold standard for planning out the surgery. Can range upwards of $1200. Learn more: dodgerslist.com/2020/05/23/imaging/FIND A SURGEON 1) Look for board certified neurosurgeon (DVM, ACVIM (neurology) OR.... 2) Look for a specialist surgeon (DVM, ACVS) who has done not just ortho (bone related) cases but a good number of neuro cases as well. Use this directory to find these specialists: find.vetspecialists.com Look through the Forum's directory for member recommendations: dodgerslist.boards.net/board/13/member-reported-surgery-costs-recommendationsLook into Care Credit now just in case things go into crisis mode and surgery is needed. It is best to know all your options, financially and where surgery would be done, ahead of time rather than scrambling for that information in an emergency. No or low interest credit for veterinary costs can be obtained from Care Credit. You find out online if you qualify: www.carecredit.com/faqs.htmlSurgery vs. conservative information: dodgerslist.com/2020/02/10/surgery-vs-conservative/Body movement during sleep such as twitching, legs moving are likely dream inspired. Unless these sleep movement cause him to wake and show you signs of pain :yelping, reluctant to move, uses eyes only rather than turn head, etc. |
|
|
|
Post by Ken & Fergie on Jul 28, 2021 21:47:39 GMT -7
Thank you so much for the invaluable information. I wanted to ask about lifestyle changes after healing from a cervial IVDD for both medical and surgical approaches. I have heard that dogs must avoid jumping, going up and down stairs, and rough plays for the rest of their lives. Boy is a high energy dog who loves running, fetching, rough playing with my other two dogs, rolling in the grass, etc. And from what I have learned, there is a high recurrence rate with the conservative approach. Any reinjury requires surgery, is that correct? Also I have that once scar tissue has already formed, prognosis is 25% less favorable.
|
|
PaulaM
Moderator.    Member since 2007: surgery, conservative . Montana, USA
Member since 2007: surgery, conservative . Montana, USA
Posts: 19,528
|
Post by PaulaM on Jul 29, 2021 6:31:28 GMT -7
Ken, do you have a diagnosis from your vet that BoyBoy was born with a premature degenerative disc disease called intervertebral disc disease? We have been prudently assuming this is a disc episode until you had a vet diagnose what Boy is suffering from. Most disc episode cases are diagnosed by the way the dog acts (symptoms) at the exam, past history of disc pain, the breeds prone to this disease and the hand's on neuro exam. If a vet is suspicious of another disease, an x-ray could help to rule it out. X-ray because they only show boney hard tissue can not prove a soft tissue disease of discs and spinal cord. The only disease we have a lot of experience with is IVDD. So while you are prudently acting as if this is a disc episode until you have a diagnosis from a vet, these answers are for the disease of IVDD. Dogs born with the genetic disease IVDD can have any of the neck or back discs prematurely degenerate enough to bulge, tear and herniate into the spinal cord canal. Vertebrae illustration The neck C1-7, Chest T1-13, the low back L1-7 Changing life style a bit is to try to prevent or lengthen the time til a disc episode happens. -- Keep your dog slim with an appropriate weight to take stress off the back -- Strengthen the core muscles which support the spine with swimming, running, long walks. -- Avoid exercises that include jumping up or down, zig zag running with abrupt stopping. -- Encourage games and activities that include nose work, hide and seek. -- Avoid kill the prey type of activity that involves shaking the head. IVDD is a unpredictable disease. Some few dogs have their first disc episode at age 1. Typically it is not until the dog is 4-7 years old, with the first signs of pain, the vet and owner know the dog was born with IVDD. Some dogs have only one disc episode their entire life. While others may have multiple disc episodes. The two treatments seek the same outcome of taking pressure off of the spinal cord (decompressing the cord). -- Surgery does this by physically removing bits of disc material where it is not supposed to be (inside the spinal cord canal). -- Conservative treatment decompresses the spinal cord with an anti-inflammatory drug and the hope disc material will shrink back (be absorbed by the body) from the cord. The disc itself self heals under conservative treatment of 8 weeks of limited movement. With surgery some of the disc material inside of the disc had escaped and was physically removed. This makes is far less likely for this same disc to have another problem. But the same surgical disc has in some cases torn again causing pressure to the cord. The usual reasons for a surgery are: -- If the dog can’t walk OR with STRICT crate rest, neurological functions worsen and are lost (leg movement and bladder control). -- STRICT crate rest is employed and after several attempts to go off of the anti-inflammatory, pain returns. -- If 100% STRICT crate rest has been employed and pain medications have been adjusted (dose, frequency, and mix of pain relievers), but the pain can’t be brought under control. -- If a dog is experiencing similar signs of neck or back pain, or mild neurological deficits for the 3rd or 4th time, meaning it may be the same disc is involved. SCAR TISSUE -- The disc itself forms scar tissue. That is a good and desired thing. -- The cord itself could form lesions (scar tissue) where the escaped disc material has been touching the cord for some time. That may not be a good thing. It makes it harder for the surgeon to remove the disc pieces. The surgeon may not be able to then remove 100% of the disc material for fear of damaging the spinal cord. This Forum started in 2002. We have owners who update us a year or several years out from the disc episode. Most surgeons do not have contact with the owner much beyond the last check up visit at 4-6 weeks. From our advantage point we've noticed many dogs do not get those memo's about percentages of things going to happen. Dog with high percentages of never walking again, go on to walk. Dogs given percentages of going to have another disc episode, never have another in their long lives. All we can say to owners is know your dog's disease. Be prepared to act quickly when seeing the signs. Crate at once to protect the cord. Get to a vet asap for a diagnosis and the corresponding treatment..
i1.wp.com/dodgerslist.com/wp-content/uploads/2020/03/SIGNSepisode.jpg ** Upon completing the treatment for a diagnosis of disc disease and graduation from the weeks of rest, we will have lots of information to share with you to reintroduce Boy back to family life and activity. Things like disc friendly games and activities and making your home back friendly plus training for Boy. Life will go on with the new normal.
I hope this helps your mind sort things out.
Do let us know if you have received a diagnosis. What is the name given to the disease Boy has? |
|
|
|
Post by Ken & Fergie on Jul 31, 2021 0:18:51 GMT -7
We have yet to confirm a diagnosis but my vet thinks it's cervical hyperesthesia and referred me to a neurologist. So as you suggested, I am treating it like a neck slipped disc, considering the fact that the yelping started only after his dental procedure.
He has intermittent yelping, muscle tremor, low head carriage and root signature sign. Other times, he acts normal. Is root signature sign considered nerve deficit and therefore be categorized as grade II or is root signature sign a symptom of pain (grade I)?
I think Boy is feeling better. He has not yelped in two days, though I think sometimes there is still some discomfort and/or anxiety, i.e lip licking, panting, and trying to reposition.
Unfortunately, I was still letting Boy jump up and down the couch, use the stairs, and go on walks after he returned from his dental procedure on 7/20, which is when the yelping began. I have only started to try to keep him quiet on 7/24.
Here is Boys regimen:
The first week: (July 26- Aug 2)
1. Galliprant 60mg 1x day
2. Gabapentin 300mg 3x day
3. Methocarbomol 500mg 3x day
The second week: (Aug 3- 10)(lowered dosage)
1. Galliprant 60mg 1x day
2. Gabapentin 300mg 2x day
3. Methocarbomol 500mg 2x day
The third week:
Stop Methocarbomol first, then taper off Gabapentin. According to my vet, Galliprant is safe for long term use. He did not recommend steroids.
[Moderator's Note. Please do not edit
65 lbs 10 y.0.
Galliprant as of 7/19: 60mgs 1x/day for TBA days, then TEST STOP for _ pain/_neuro
crate rest 7/24 start
Gabapentin 300mg 3x/day; 8/3 will be 2x/day; 8/11 further back off to stop
methocarbamol 500 mgs 3x/day ; 8/3 2x/day; 8/11 stop
needs GI tract protector, Pepcid AC, on board w/Galliprant! ]
Boy is on "room rest" but someone is with him 24/7 to make sure he does not move his neck too much.
Four potty breaks per day, carried up and down stairs.
Elevated food and water bowl.
Boy will be seeing a resident vet/neurologist at UC Davis on Aug 10. I know that one of the members here recommended UC Davis. I am guessing surgeries are done by students with supervision of teachers. I also have an appointment with a neurologist on Aug 19 at another clinic. Boy does not show symptoms until there is a flare up, so what should I expect during the consultation? Is it better to see two neurologists?
I have only been doing homework on conservative treatments and prognosis and have yet to look too deeply into information regarding surgery, which I hope I can avoid.
Thank you.
|
|
PaulaM
Moderator.    Member since 2007: surgery, conservative . Montana, USA
Member since 2007: surgery, conservative . Montana, USA
Posts: 19,528
|
Post by PaulaM on Jul 31, 2021 10:32:02 GMT -7
Good to hear no signs of pain (yelps) now for two days! With a disc episode pain on the stop of Galliprant, any pain meds, would be a signal that not all the swelling is gone. More time back on Galliprant and the original doses of pain meds are used. Then another test stop of Galliprant and pain meds. I know your vet is not calling for a test stop of Galliprant at the same time pain meds are backed off. This can delay finding out the true nature of any existing pain. Rule of thumb is:
pain = swelling = more time on
non-steroid anti-inflammatory (Galliprant NSAID)
pain meds and Pepcid AC needed. Always have a plan "B" in place with the vet during a test for pain stop on what you should do should pain surface. Have enough meds on hand should that happen over a weekend or evening when the Vet is closed, to save an expensive ER visit.There is a presumed disc episode that is going on at this time and that would take 8 weeks of limited movement to heal the disc itself. Things that could cause pain to surface could be: moving too much (transports, restricted area too large), reduction of pain meds, test stop of Galliprant, and if the supposed disc material can shift some it could maybe cause more or less pain to the peripheral nerve. With a supposed peripheral nerve being pinched by disc material, that causes pain. If supposed disc material would instead be pushing on the actual spinal cord, that could cause both pain and if enough pressure to the cord cause neuro function diminishment. What are the details surrounding when pain resurfaces for Boy during this assumed disc episode? Details of dates, time of day, what he had been doing or was doing are all helpful details for the vet and us in figuring out things. Are you keeping a med chart to make notes on... very useful to see patterns, have dates and specific facts handy as you discuss things with the vet. dodgerslist.com/wp-content/uploads/2020/02/med-chart-printable.pdfVeterinary residents at a private practice or a university are there for course work and training. These DVM vets have a supervising board certified neuro (DVM, ACVIM) or an ortho surgeon specialist (DVM, ACVS) during surgeries, etc. It will be good to finally have a diagnosis on Aug 10 to follow an appropriate treatment for Boy's problem. |
|
|
|
Post by Ken & Fergie on Jul 31, 2021 11:57:01 GMT -7
Yes I am keeping track of his symptoms and time of flare ups
7.20 whining after anesthesia. Not eating until 5pm.
One of the rear leg gave out slightly when walking (can be due to anesthesia still in the system)
Yelped twice at night when I was moving him by the front legs while he was lying down.
7.21 still subdued. Doesnt want to make fast movement. Hesitant head shake only, not body like before. Yelped lightly once when walking to potty.
7.22 Yelped loudly when he tried to get up in the morning while lying on his side. The right rear leg seems to gave out a bit and he immediately lied down. But no limping afterward.
Yelped again when getting up later
7/22 More energy. Yelped loudly when coming to the door to greet me.
I then called the vet who thinks it's back pain and recommended 2-3 wks of rest. At that time, I thought it was a sprained back. The vet did not offer any pain meds. Only said if it's pain only, ok to monitor until Mon to see him. If lameness in the legs, take him to ER with neuro on staff.
7/23 middle of the night yelped
Morning yelped when sliding off the dog bed. Tried to stand up back leg gave out a bit.
During walk my ankle hit his jaw slightly and he yelped
When sitting down, I tried to lift his head and he yelped
Head lowered
This is when I noticed he is not putting weight on front right leg. Lip licking.
7/24 morning struggled to get up. gingerly movement. I assume he is afraid to move a certain due to pain.
3pm Yelped when getting up
Pain is intermittent, usually after lying in the same position and trying to get up
Was able to look up, turn neck around, still lifting rear legs to urinate without issues.
5pm sleeping not moving and yelped
When on walk, seems to return to normal
I asked for some pain meds and got Galliprant.
11pm light yelp getting up after napping for a while. Front right left lifted. Back to normal
I also noticed right neck chest muscle tremor.
[7/24 Restricted Movement rest started]
7.25 made it through the nigh without hearing yelping. But he seems to be gingerly at times
Morning 10:30 after lying down for a while, got up no problem but gingerly. Lip licking wont raise head. Right foot more elevated
2pm yelped while sleeping in bed. Then tried to walk around (restlessness), lip licking. Tail is tugged
8pm yelped loudly. Jumped out of bed.
9PM get up too fast yelped loudly, right front leg lifted up. Panting.
10pm sleeping position tried to get up. Yelped.
7/27 Yelped loudly twice when trying to get up from lying sideway.
7/28 Yelped lightly once. Panting at night. A bit of restlessness.
7/29 Yelped lightly once getting up
7/30 no yelping but lip smacking after getting up (nervousness), weakness front right left. Maybe rear right leg, also, not sure.
7/31 no yelping. Neck shivering when was outside peeing. Could be the cold weather. Or a setback after head shaking. But returned to normal when he's back inside.
He was acting normal at the vet. Excited to see new people. There is no reaction upon neck/back spine palpation.
PATTERN: Yelping usually is triggered when getting up from a sleeping position.
Neck seems to be the culprit because of root signature and low head carriage.
The vet said as long as he's poop is normal and he's eating fine, there is no need for ✙Pepcid AC , but he said I can give it to him 20mg per day as I see fit. I have purchased it.
[Moderator's Note. Please do not edit
65 lbs 10 y.0.
Galliprant as of 7/19: 60mgs 1x/day for TBA days, then TEST STOP for _ pain/_neuro
crate rest 7/24 start
Gabapentin 300mg 3x/day; 8/3 will be 2x/day; 8/11 further back off to stop
methocarbamol 500 mgs 3x/day ; 8/3 2x/day; 8/11 stop
✙Pepcid AC 20 mgs 2x/day
8/10 Neuro appt]
I have asked for extra pain meds.
Thank you.
|
|
|
|
Post by Romy & Frankie on Jul 31, 2021 13:37:35 GMT -7
You have done a good job keeping a detailed watch on Boys symptoms and what seems to exacerbate pain.
I am very glad that you have asked for a change in pain meds. I know that Boy has not yelped so far today but If he continues yelping it is a sign of pain. Neck disc issues are particularly painful. Boy should not be in pain. Vets have many ways to address pain.
Some Dogs instinctually try to hide pain at the vet or in other situations where they feel insecure. The fact that he did not show pain at the vet but has shown signs of pain at home may be due to that instinct.
The lip smacking may also be a sign of nausea. The Pepcid AC will help with any nausea Boy is feeling, so please start it right away. |
|
|
|
Post by Ken & Fergie on Aug 3, 2021 16:59:04 GMT -7
Hello I just learned that there are two types of IVDD: Hansen Type 1 and 2. Is a definitive diagnosis made only by Xray or advanced imagining? I read that Surgical vs. conservative management have similar outcomes for Hansen Type 2 bvns.net/wp-content/uploads/2017/03/IVDD-Facets-2017.pdf |
|
PaulaM
Moderator.    Member since 2007: surgery, conservative . Montana, USA
Member since 2007: surgery, conservative . Montana, USA
Posts: 19,528
|
Post by PaulaM on Aug 3, 2021 17:28:51 GMT -7
Ken, small breed dogs with short dwarfed legs are likely to have Hansens I. Dogs with these discs tend have a disc episode that happens fast in a matter of a couple of days or couple of hours. The gene that makes their legs dwarfed may also be the cause of prematurely aged discs. The disc cartilage hardens and can bulge, tear when the vertebrae move and push on the no longer cushiony disc. The most typical age for owners and the vet to first learn the dog was born with this disease is 4-7 years old. Can happen earlier such as age 1 or older than 7 y.0.
These are the typical breeds (not a complete list):
Australian Cocker Spaniel, Coton de Tulear, Pembroke Welsh Corgi, Australian Shepherd, Dachshund
Pinscher (miniature), Beagle, Dandie Dinmont Terrier, Poodle (miniature and toy), Bichon Frise
French Bulldog, Pug, Boykin Spaniel, German Hound
Rat Terrier, Bulldog, Havanese, Scottish Terrier, Cardigan Welsh Corgi
Jack Russell Terrier, Shih Tzu, Cavalier King Charles Spaniel
Lhasa Apso, Skye Terrier, Chihuahua, Maltese, Yorkshire Terrier, Chinese Crested, Pekingese
We've had on this Forum some large breed dogs which have been diagnosed by a neuro and had surgery.
Large breed dogs tend to have Hansens II. These discs age because of the natural aging process. Tends to be a slow and gradual thing.
The only way to look at soft tissue of discs and of spinal cord is with advanced imaging (MRI is the gold standard, CT, or myelogram.
No disc episode is every proved by an x-ray, it might give a suspicion but no proof.. X-ray's are used to rule out other disease that mimics a disc episode (vertebral fracture, bone infection, tumor, etc.) X-rays only show hard tissue.
I'm glad you have a neuro appt set up on Aug 10 just around the corner. Boy definately needs a diagnosis where there then will be specific things you and the specialist can discuss about the treatment.
Can you update us on how Boy is doing today with moving his neck, pain, etc?
|
|
|
|
Post by Ken & Fergie on Aug 3, 2021 21:06:14 GMT -7
Thank you Paula. Boy seems to be doing better the last couple of day, i.e no loud yelping (light whine once or twice when getting up in the last three days), no root signature signs. He is not tentatively shaking his head now and there is no ginger movement like before. I stopped ➖ Methocarbomol [8/3] today. But every time he gets up, he licks his lips. I am not sure if this is a habit of his or if it's a sign of discomfort / anxiety.
[Moderator's Note. Please do not edit
65 lbs 10 y.0.
Galliprant as of 7/19: 60mgs 1x/day for TBA days, then TEST STOP for _ pain/_neuro
crate rest 7/24 start
Gabapentin 300mg 3x/day; 8/3 will be 2x/day; 8/11 further back off to stop
➖ methocarbamol 500 mgs 3x/day ; 8/3 2x/day; 8/4 stopped
Pepcid AC 20 mgs 2x/day
8/10 Neuro appt]
I am worried that he has Hansen Type II which has a poor prognosis for surgery. Also I have read that conservative treatment for cervical is not as effective.
Since he only started yelping after his dental cleaning. I am almost certain his neck was manipulated during anesthesia which triggered the symptoms, because Boy has never yelped before. He was fetching the day before. It can rule out many other diseases that resemble IVDD, is that correct?
I would much rather doing an MRI and skip Xrays to avoid radiation/ more sedation.
MRI in my area costs $4000 to $6000. Animal Scan is charging $2100 for only one part of the body, ie head, neck, back. What would be the wise thing to do?
Also, is it better to get an MRI as close to surgery date as possible? Can I get an MRI for Boy now, but wait to do surgery months later?
Thank you again. I am truly glad I came across this site with such invaluable information.
|
|
PaulaM
Moderator.    Member since 2007: surgery, conservative . Montana, USA
Member since 2007: surgery, conservative . Montana, USA
Posts: 19,528
|
Post by PaulaM on Aug 4, 2021 8:50:55 GMT -7
Ken, you report pain healing is going in a good direction. This may well be proof that the care (meds, rest) you are giving is woking. So maybe this is a disc episode. Final proof the care has worked is at the full stop of Galliprant and all pain meds and no surfacing of pain.
California prices have alway been high. It appears if an MRI is needed the issue is in the neck. IF a neuro is suspicious that another disease is the cause of the neck problem, then less expensive x-ray may well be able to rule out those other things. Always be up front on your financial ability with the neuro. Most disc episodes are diagnosed by the dog's history, the way they act at the exam. Local vets don't have MRIs in their clinics and x-rays don't proove a disc episode.
-- MRI for a surgery would need to be done again right before the surgery to plan for the procedure with current info in hand.
-- An MRI 8/10 would be because the neuro has suspicion there may be something else going on that that an x-ray suggested. He would then want to see more clearly. IF the neuro, based on history facts you present, the good progress about pain, the neuro exam, feels this is a neck disc and the pain was/is likely root signatures he might just say continue to the conclusion the medication regime.
-- The neuro consult then is to confirm you are proceeding correctly with current care and meds treatment your own vet was not in an IVDD comfort zone to do.
With Boy progressing nicely on the stop of one pain med, and if pain continues to not surface on the stop of the another pain med and the stop of Galliprant, then a surgery is not seemingly indicated at this point in time .
Best to not jump the gun on worrying/surgeries. This whole issue is because your local vet was not comfortable in giving you a diagnosis. A span of time since 7/19, is showing what you are doing is likely resulting in good reduction/elimination of pain. The neuro consult can give you the info you need and peace of mind to help in living many happy years ahead with Boy.
|
|
|
|
Post by Ken & Fergie on Aug 4, 2021 17:08:00 GMT -7
Thank you. My vet said to taper off Gabapentin but did not provide specific instructions on how to do so. I contacted him but he is out of town for the week. He's been on 300mg 3x per day for 7 days. Should I do 2x a day for 3 day, then 1x a day for 3 days, then every other day? What is the best way to go about it? Thank you.
|
|
PaulaM
Moderator.    Member since 2007: surgery, conservative . Montana, USA
Member since 2007: surgery, conservative . Montana, USA
Posts: 19,528
|
Post by PaulaM on Aug 4, 2021 17:37:51 GMT -7
Your vet Rx'd Gabapentin 300mg 2-3x per day. So you could go to 300mg 2x/day for a couple of days. By then you may be able to contact your vet for further instructions. The Mar Vista vet webpage had a very good directory on medications. You may learn something there : www.marvistavet.com/pharmacy-center.pmlDirect gabapentin link: www.marvistavet.com/gabapentin.pmlOnly steroids need the every other day dose to signal the body to make its own steroid hormone again. |
|
|
|
Post by Ken & Fergie on Aug 10, 2021 21:23:30 GMT -7
Just a quick update after Boy's consultation with a neuro at UC Davis:
The vet examined Boy and did not find any neurological deficits. Due to Covid, I was not allowed in the exam room. What does the exam usually entail?
She did not recommend any diagnostic tests since Boy seems to be doing fine after a few weeks of conservative treatment. She suggested stopping all pain meds and monitor for relapse, and bring him back if symptoms return.
[Moderator's Note. Please do not edit
65 lbs 10 y.0.
Galliprant as of 7/19: 60mgs 1x/day for 23 days, then 8/11 TEST STOP for: _ pain/_neuro
crate rest 7/24 start
Gabapentin 8/3 will be 2x/day; 8/11 further back off to stop STOPPED 8/11
Pepcid AC 20 mgs 2x/day STOPPED 8/11
8/10 Neuro appt: test stop all meds]
She also said it might be a neck muscle sprain/strain instead of IVDD. It would be impossible to tell without advanced imaging. Apparently, soft tissue injuries can also cause root signature signs (?). Though I was certain that Boy's symptoms were consistent with cervical IVDD.
She suggested another two weeks of rest, then [8/24] slowly introduce controlled, leashed walking 2-3 times a day starting just 5-10 min and build up from there. No stairs, jumping on/off couch and bed, and no strenuous exercises.
I have another neuro appt at another clinic in 10 days. Is a second opinion necessary in this case or should I cancel?
Thanks again for all the support and guidance.
|
|
PaulaM
Moderator.    Member since 2007: surgery, conservative . Montana, USA
Member since 2007: surgery, conservative . Montana, USA
Posts: 19,528
|
Post by PaulaM on Aug 11, 2021 7:38:14 GMT -7
Ken, too bad you were not allowed into the exam room. That is where you can learn much in just watching. This article is for veterinary graduates goes over the details of giving a NEUROLOGICAL ASSESSMENT exam. If you stop all meds today 8/11 (pain med gabapentin + anti-inflammatory Galliprant), then you should have a quick ability to observe for pain. You never reported any neuro diminishment so would expect on the test stop of all meds you would not see any beginnings of neuro issues surfacing (nails scuff floor, wobbly walking, paws knuckling under). It takes pain meds to 8 hrs to clear the body and it can take 5-7 days for Galliprant to clear the body. So days well before the 2nd neuro appt 8/21 you should have observations (if they are to surface) for the neuro to observe for himself in diagnosing. If are not seeing any neuro or pain issues, then there is nothing for the 2nd neuro appt person to work with in diagnosing. You'd cancel the appt. Then with no ranked diagnosis, it is YOU who will then have to decide for yourself, if it is prudent to act as if this might likely be a neck disc episode that caused the front leg issues (you did not get a ranked diagnosis if IVDD higher than muscle sprain). IF you prudently decide it might be disc related as top ranking, then you'd want to be sure Boy got the full 8 weeks for the disc to heal and not start any physical PT (going on 5-10 min walks). If it would be a neck disc, then the single most important care is getting the disc to heal with STRICT rest with a target date of Sep 18 graduation day. DIAGNOSIS "Differential diagnosis is a process of formulating, and ranking, educated guesses as to cause. This in turn guides diagnostic testing to confirm or rule out specific diagnoses." Fingeroth, DVM, DACVS. January 2006 Surgery. dcavm.org/06jan.html Last accessed 2014---- "Intervertebral disc disease (IVDD) may be strongly suspected on the basis of clinical signs especially in predisposed breeds, however, diagnostic imaging is required to confirm the diagnosis." Fitzpatrick Referrals. Intervertebral Disc Disease. www.fitzpatrickreferrals.co.uk/neurology/intervertebral-disc-disease/-------- Ken, we'll be very interested in what you observe with today's stop of all meds, what you observe regarding any surfacing of pain over the next 5-7 days when all meds are out of his body. 5-7 days is because depends on how fast Boy metabolizes meds, it is different for each dog. |
|
|
|
Post by Ken & Fergie on Aug 20, 2021 13:59:21 GMT -7
Boy's been off all pain meds since 8/10 and there is no evidence of pain since.
He is back to his boisterous self.
He is shaking his head and body normally like before and rolling on his back in the bed like before, both of which I can't stop him from doing. I am still restricting his activity for another few weeks just in case. I will continue to stop him from jumping. Is it safe to let him run or possibly play fetch?
|
|
PaulaM
Moderator.    Member since 2007: surgery, conservative . Montana, USA
Member since 2007: surgery, conservative . Montana, USA
Posts: 19,528
|
Post by PaulaM on Aug 20, 2021 14:46:23 GMT -7
Ken, since there is no diagnosis, it is YOU who will have to decide whether it is prudent to assume this was a disc episode and allow the suspicion of a disc episode time for the disc to complete formation of scar tissue. Graduation date from strict rest would be on Sept 11. Oophs I think last time I wrote is miscounted and wrote Sep 18. A slow transition back to activity at graduation would be so you are not confused if pain were to arise, was it temporary overdoing physical activity or was it more serious of another disc episode? This page will give you and idea of a schedule for reintroducing Boy back to family life and physical activity over a couple of months period. Might not be a bad idea to do a gradual release to physical activity even if you feel this was never a disc episode. Gives you a chance to monitor things and if pain would surface to quickly notice and crate at once, get to a vet for a diagnosis, a treatment and meds if needed for the treatment. So here is the page and it also includes back/neck friendly activities for those dogs who have IVDD: dodgerslist.com/2020/06/15/back-friendly/?highlight=sample%20schedule |
|